Maximize Your EHR Investment With Healthcare Revenue Optimization
Ingenious Med offers seamless, bi-directional integration with your EHR, including Epic and Cerner, extending your EHR’s capabilities and strengthening your revenue with comprehensive charge capture.
Our charge capture platform uses AI-powered prompts and real-time automation to help providers surface missed charge opportunities directly within the clinical workflow. In fact, our research shows that without AI, 13% of all charges are under-coded and 7% are over-coded.
The automated prompts ensure coding compliance and empower providers to capture accurate charges at the point of care on any mobile device. By automating charge reconciliation and flagging inconsistencies, our clients reduce denial rates and significantly improve revenue integrity.
Solving Common Revenue Cycle Optimization Issues with Mobile Automation
Our mobile-first approach means meeting providers where they’re at, alleviating the administrative burden on healthcare providers. This means charges entries won’t be delayed until the end of a shift where accuracy can drop and charge lag increases.
Instead of batching charges at the end of the day, providers capture billable services instantly at the point of care from any device. This eliminates administrative tasks from their day and enhances patient satisfaction. AI-powered prompts drive real-time coding compliance and revenue cycle management. Automatically surface coding requirements and flag inconsistencies before claims reach the billing office.
Critical Features of Hospital Revenue Cycle Management Software
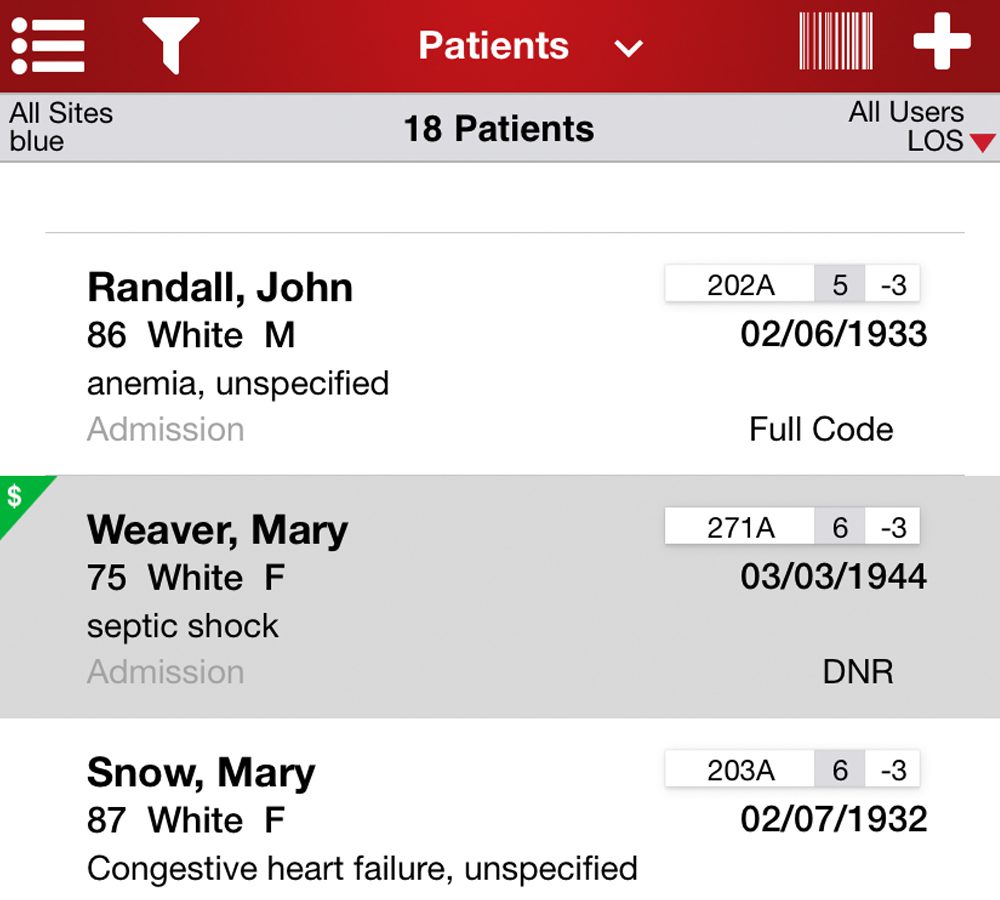
Comprehensive Charge Capture for Revenue Optimization
- Track all patient care episodes via real-time census and appointment data feeds.
- Capture charges easily and accurately across any acute, SNF, or other post-acute location.
- Lighten clinician workloads with automatic prompts and intelligent code filters.
Improved Coding Compliance
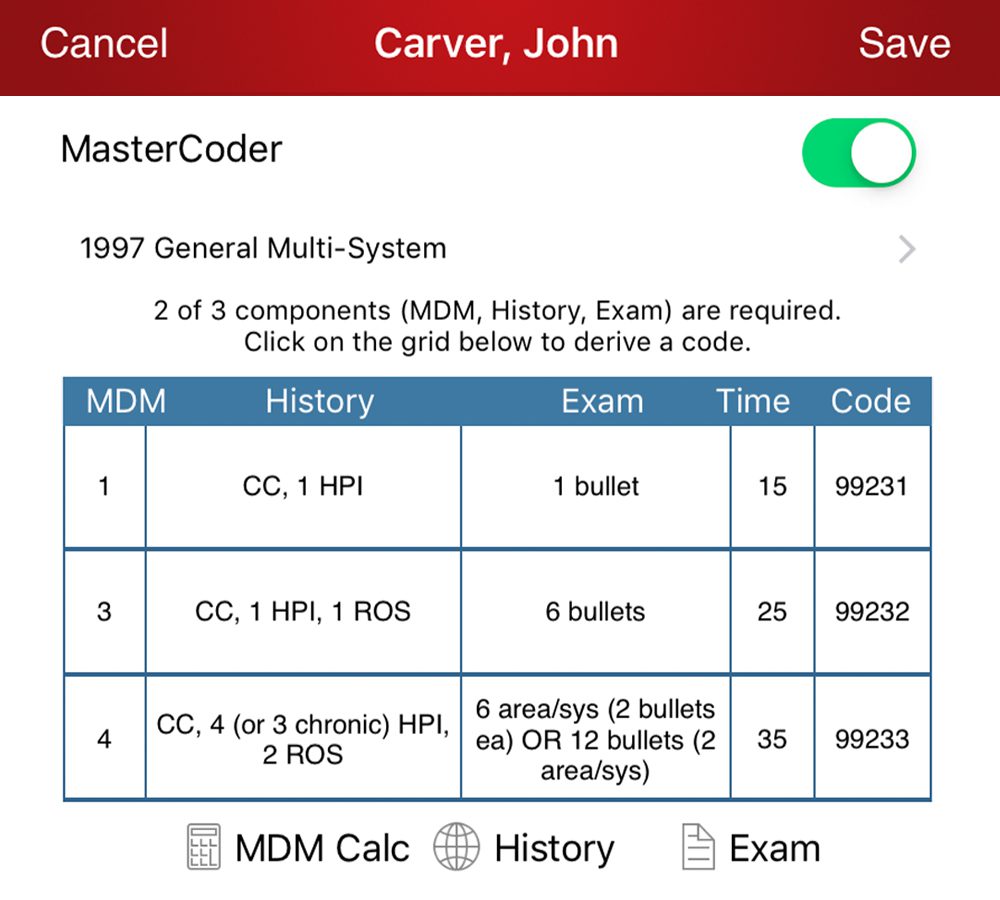
- Improve coding speed, accuracy, and compliance with MasterCoder — a step-by-step tool that reduces coder workload.
- Avoid denials that cost your organization time and money.
- Reduce reimbursement turnaround times so you can plan more accurately.
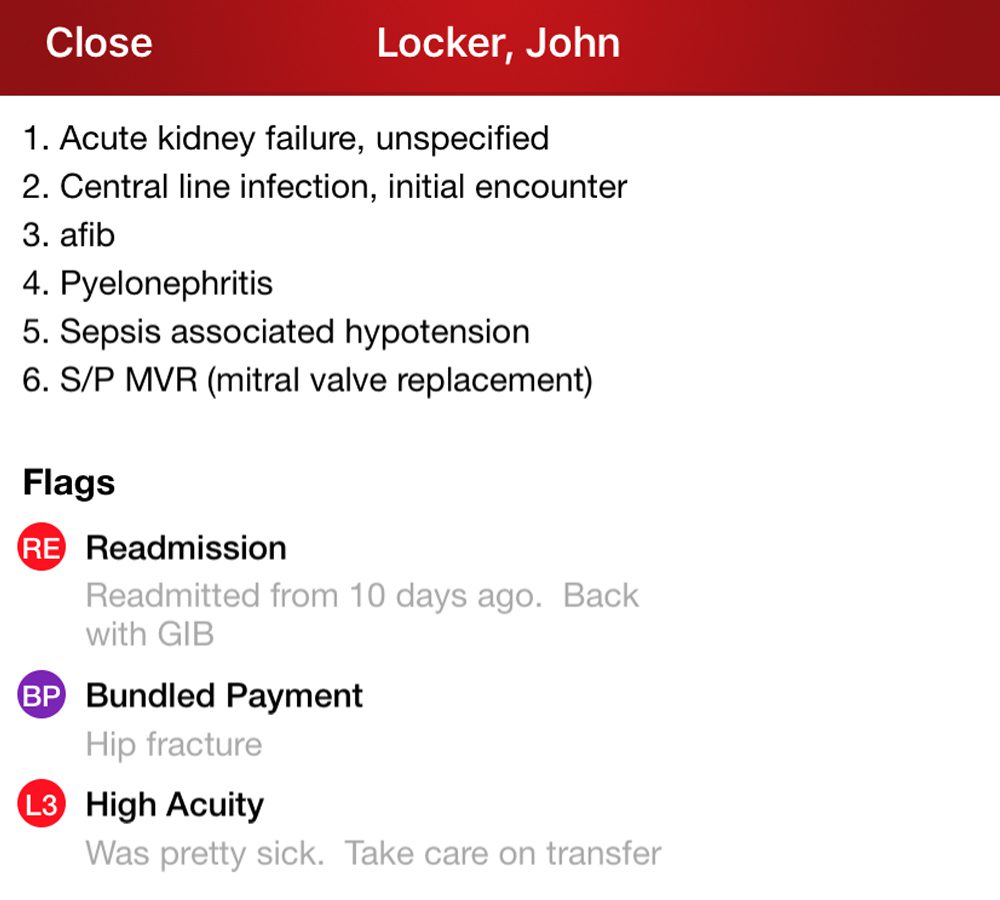
Value-Based Metrics Management
- Simplify MIPS submissions to gain additional incentives and avoid penalties.
- Automatically identify members of value-based programs such as BPCI, ACOs, case rate and more.
- Save costs and manage patient throughput using our length-of-stay indicator and customizable flags to avoid discharge delays, manage care transitions and reduce readmissions.
Stronger Revenue Integrity
- Automatically confirm substantiating EHR documentation with Charge Note Reconciliation.
- Alert providers to possible missed bills through in-platform chat, visual indicators, and push notifications.
- Automatically identify and prevent missing charges based on clinical documentation feeds.
- Assign missed encounters to the providers responsible with one click.
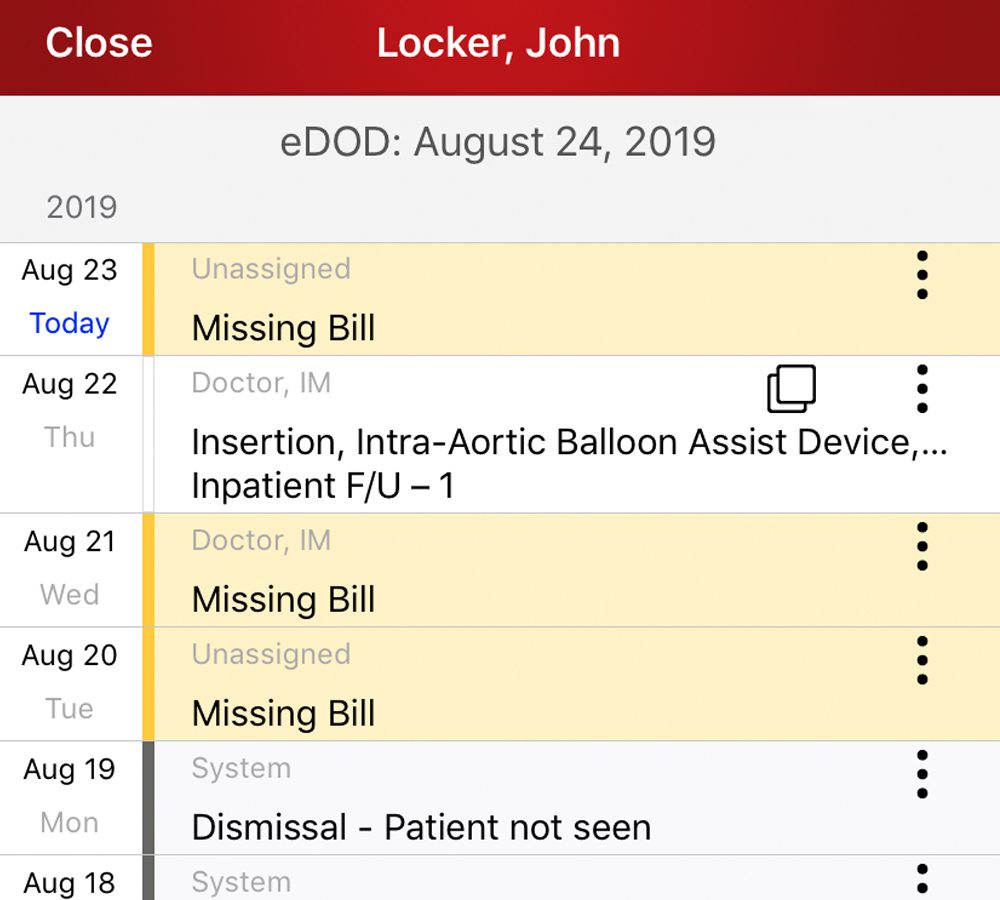

Charge Note Reconciliation
Physicians work under constant time pressure, which can sometimes lead to incomplete charge capture for patient encounters. This may be due to:
- Missed Charges — Not capturing all billable services during patient encounters.
- Unsigned Clinical Notes — Incomplete or unverified record.
- Misaligned Documentation — Charges do not reflect the documented level of service.
Charge Note Reconciliation and Document Viewing integrate directly within the Ingenious Med platform, offering Real-Time Charge Reconciliation and Integrated Document Viewing.
Take the Next Step in Revenue Integrity
Achieving lasting revenue integrity requires dedicated, intelligent tools — not just “good enough” software. The Ingenious Med charge capture system offers a proven, risk-adjusted path to revenue certainty and time recovery. See your potential recovery numbers now with our Revenue Optimization Calculator and request a demo to see how Ingenious Med integrates with your existing EHR.
